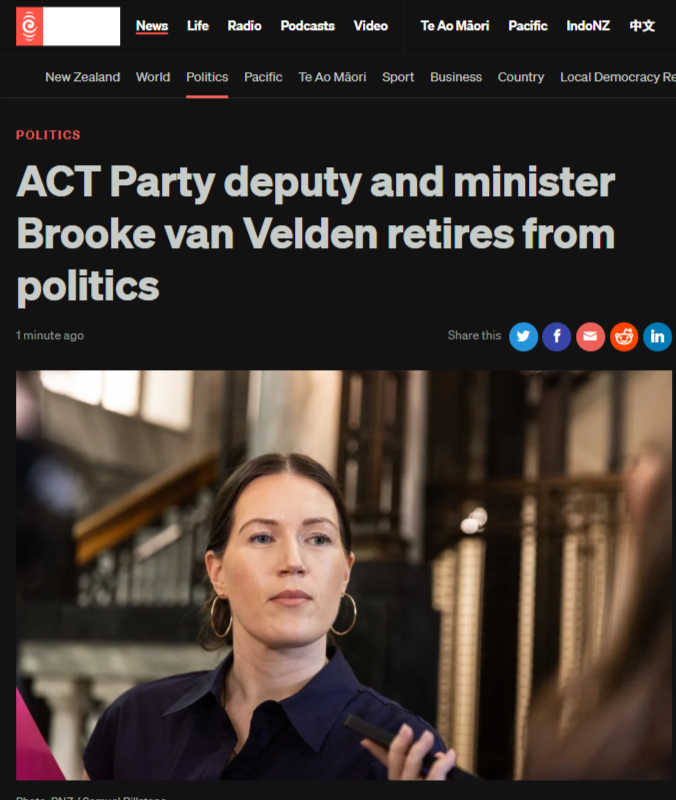
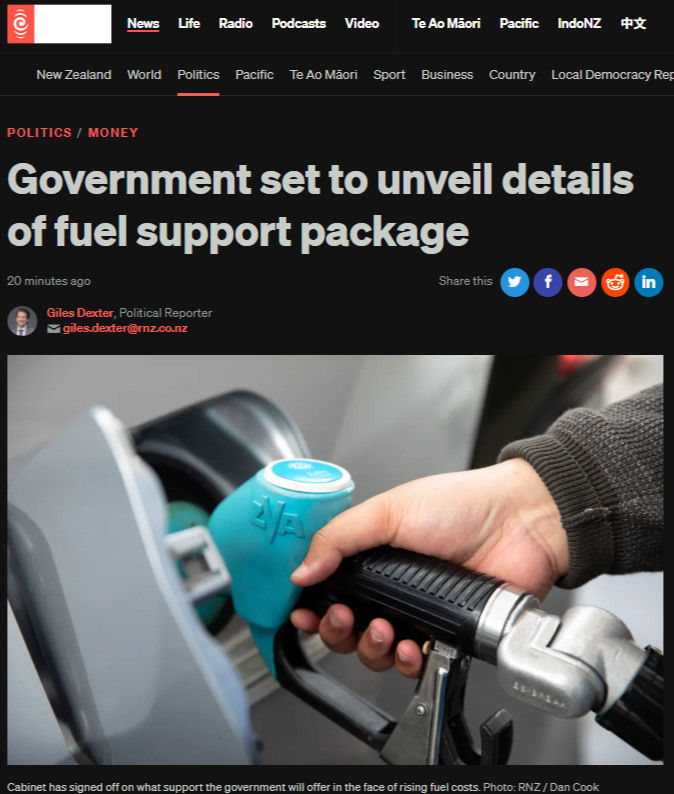
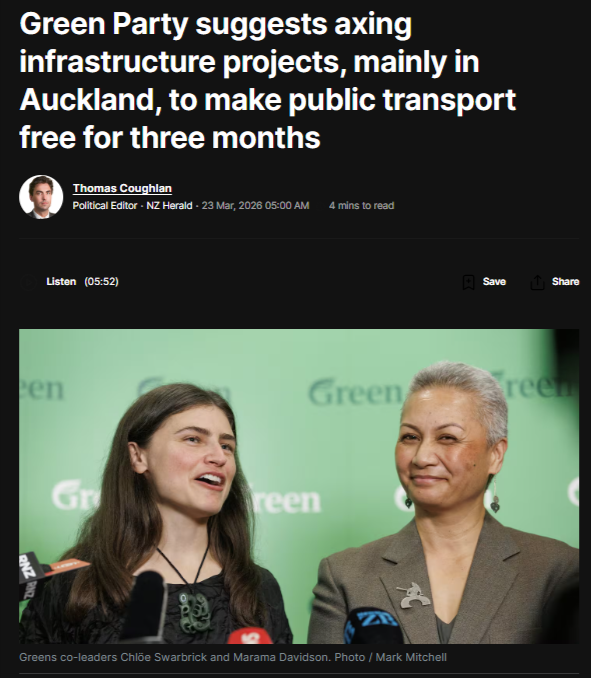
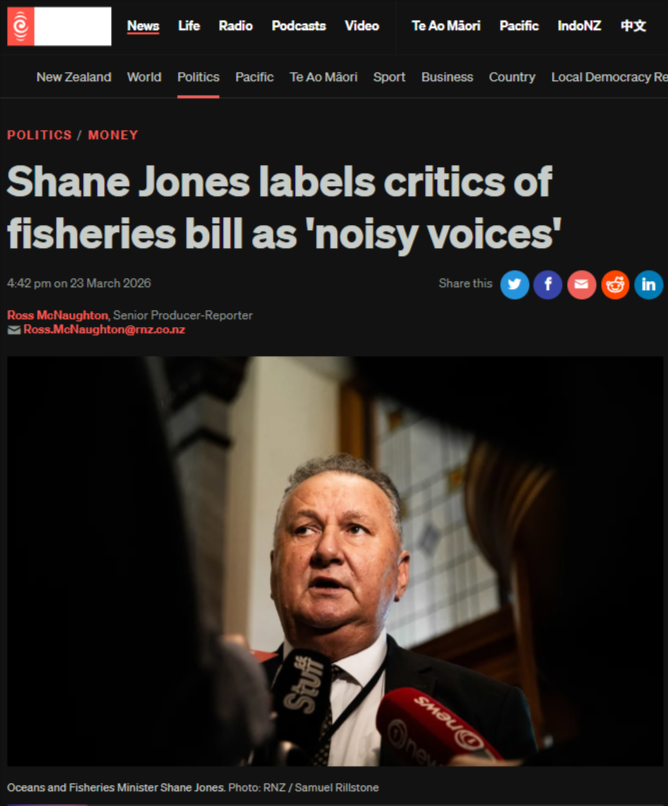
“The 140-Bed Con” - 2 November 2025
How Neoliberalism Dismantles Public Health While Buying Politicians
Tēnā koutou katoa,
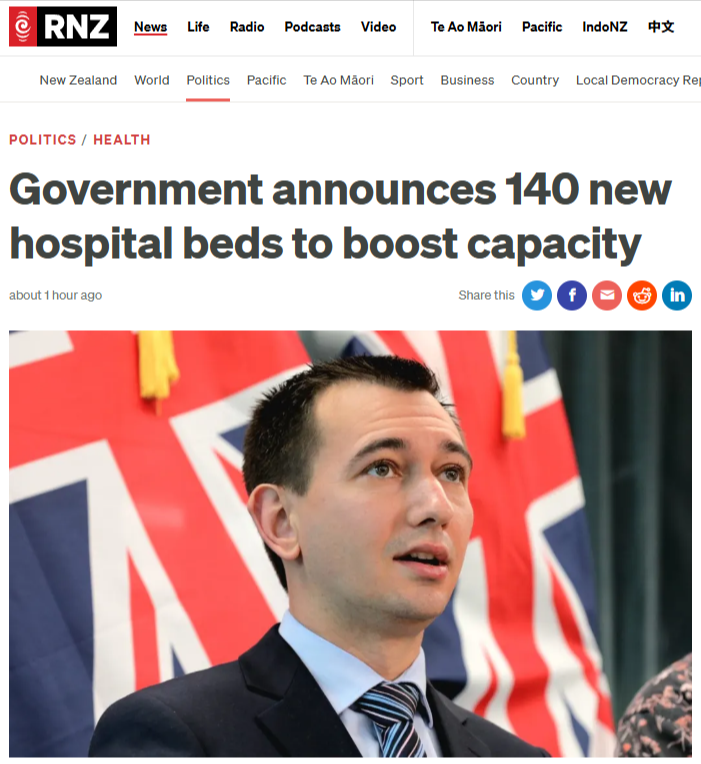
The Coalition Government announces 140 new hospital beds like a landlord offering a band-aid for a broken leg. Health Minister Simeon Brown’s November 2025 declaration of “rapid build” wards at Middlemore, Waikato, Wellington, Nelson, and Hawke’s Bay hospitals—set to open in the second half of 2026—reveals everything you need to know about this Government’s priorities: theatrical gestures over genuine solutions, private profit over public good, and neoliberal austerity disguised as pragmatic healthcare policy.
The smoking gun? While Brown celebrates 140 beds arriving in late 2026, New Zealand currently faces shortages that leave patients sleeping on floor mattresses in mental health wards and waiting 12 hours in emergency departments. These modular wards are prefabricated units constructed off-site and installed on hospital grounds, addressing a fraction of the immediate shortage while Health NZ faces a projected deficit of $1.1 billion in 2024-25, mass job losses, and systematic dismantling of Māori and Pacific health services.
This isn’t healthcare investment. It’s crisis management theatre performed by a Government that received $10.4 million in corporate donations in 2023, installed an anti-abortion activist as Health Minister, and replaced democratic health governance with a single Commissioner whose mandate includes delivering austerity.
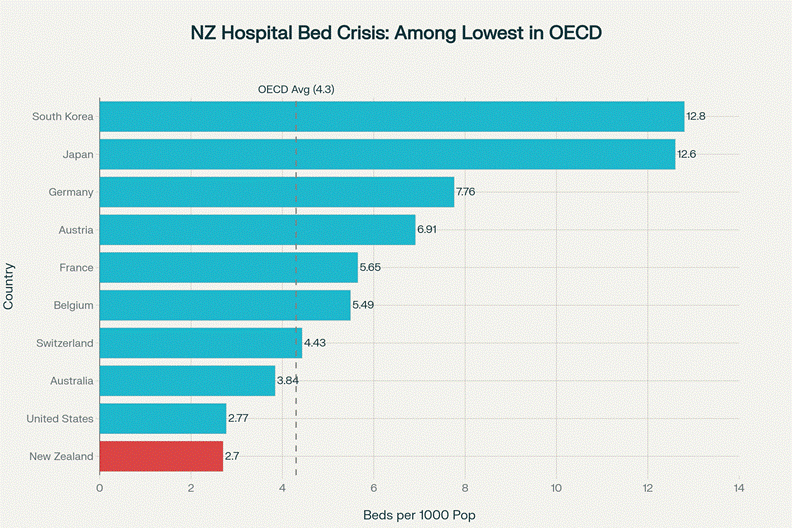
New Zealand has among the lowest hospital bed capacity in the OECD at 2.7 beds per 1,000 people, 37% below the OECD average of 4.3
The Whakapapa of Manufactured Crisis
New Zealand’s hospital bed shortage didn’t materialize overnight—it’s the culmination of decades of neoliberal policy. Researcher Bryce Wilkinson’s work has influenced both the 2001 prototype and current version of the Regulatory Standards Bill.
When National campaigned in 2023, they received $10.4 million in declared political donations, more than double any other party. ACT pulled in another $4.3 million. These aren’t disinterested civic contributions—corporations don’t pour millions into political campaigns without expecting returns measured in policy benefits.
The health system they inherited was already strained, but Labour’s 2022 reforms established Health NZ Te Whatu Ora and Te Aka Whai Ora Māori Health Authority—the most significant attempt in decades to address systemic health inequities. The Coalition’s response was surgical demolition.
Within months of taking office, they moved to disestablish Te Aka Whai Ora, eliminating dedicated Māori health leadership at the national level. By July 2024, they replaced Health NZ’s board with Professor Lester Levy as sole Commissioner, concentrating power in one individual.
The financial “crisis” they claimed justified these interventions—a projected $1.4 billion deficit—emerged suspiciously rapidly. Health NZ reported a $722 million deficit for 2023-24. The narrative shifted dramatically within weeks from assurances about fiscal management to claims of urgent crisis, suggesting manufactured urgency designed to justify predetermined cuts rather than genuine fiscal emergency.
Deconstructing the 140-Bed Announcement
What Brown Said: Five new “rapid build” hospital wards will deliver 140 beds at Middlemore, Waikato, Wellington Regional, Nelson, and Hawke’s Bay hospitals, operational by second half of 2026. These modular units will be constructed off-site and installed on hospital grounds. Brown claimed this would ease pressure on emergency departments, support faster admissions and discharges, and improve patient flow. He noted that a competitive procurement process allowed four wards to be delivered within Budget 2025 funding, alongside the Hawke’s Bay ward announced earlier.
What Brown Didn’t Say:
The Real Capacity Numbers: New Zealand has only 2.7 hospital beds per 1,000 population, compared to the OECD average of 4.3 beds per 1,000 population. This places New Zealand among the lowest-capacity nations in the developed world. To reach OECD average capacity, New Zealand would need approximately 5,000 additional beds, not 140. For intensive care, New Zealand has only 3.6 ICU beds per 100,000 population, one-third of the OECD average of 11 per 100,000.
Brown’s 140 beds address less than 3% of what’s needed to match OECD standards.
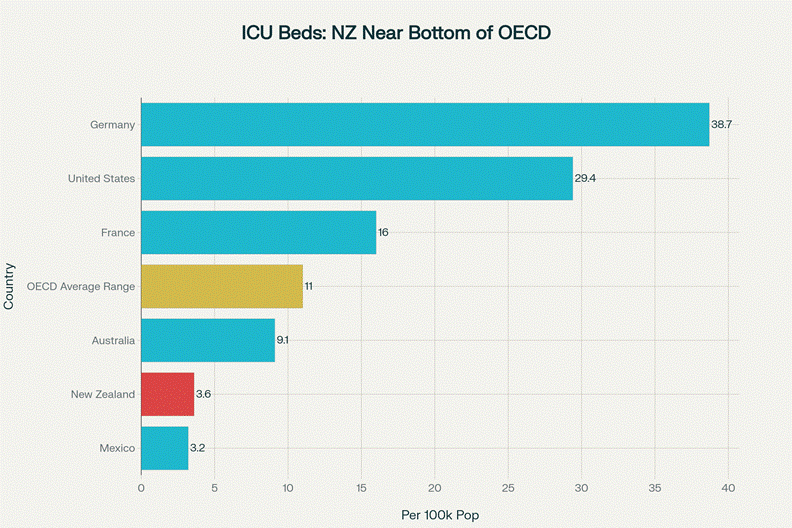
New Zealand has only 3.6 ICU beds per 100,000 people, one-third of the OECD average and among the lowest in developed nations
The Cost Secrecy: Brown refused to specify the exact funding allocated for these wards, citing bargaining position concerns. Budget 2025 allocated funding within existing health infrastructure envelopes, but the precise amount per ward remains undisclosed. This makes independent cost-effectiveness analysis impossible.
The Timeline Reality: Announcing beds in November 2025 for delivery in late 2026 means sick New Zealanders will wait 12-18 months while hospital overcrowding persists. Waikato Hospital mental health wards currently run at 140% capacity with patients on floor mattresses. Senior emergency department physicians describe hospital bed-block as “worst it’s ever been”. Hospital bed occupancy rates regularly exceed 100%—far above the 85% safety threshold.
The Staffing Silence: Not one word about who will staff these beds. Health NZ is currently proposing to cut 1,500 positions including 131 in Māori health and 115 in Pacific health services. Most health care workers believe these cuts are damaging services. You cannot operate hospital beds without nurses, doctors, orderlies, cleaners, and support staff—yet Brown offers infrastructure without workforce investment.
The Private Profit Direction: Health Minister Simeon Brown has directed Health NZ to accelerate private sector partnerships for elective surgeries. This creates a vicious cycle: defund public health, watch services deteriorate, then claim private sector “efficiency” justifies further privatization.
The Rhetoric Versus Reality: Neoliberal Doublespeak
Brown and his Coalition colleagues deploy classic neoliberal rhetorical techniques to obscure their agenda:
False Scarcity: They claim fiscal constraints necessitate cuts while offering other priorities different treatment. The narrative of unavoidable scarcity obscures political choices about what to fund.
Efficiency Theater: Health NZ Commissioner Lester Levy’s appointment came with claims that the organization had excessive management layers. The “bloated bureaucracy” narrative justifies cuts while potentially ignoring that healthcare administration requires sophisticated systems for coordination, compliance, and equity monitoring.
Target Weaponization: Brown sets health targets—95% of ED patients seen within six hours, faster cancer treatment, improved immunization rates—without providing proportionate resources. This creates conditions described as “set up to fail,” generating public frustration that further erodes confidence in public health.
Project 2025 Parallels: Russell Vought, author of the Project 2025 budget chapter, now leads the Office of Management and Budget under Donald Trump’s second term. Project 2025 explicitly calls for concentrating executive power and treating budget authority as control over all agencies. David Seymour’s Regulatory Standards Bill functions as New Zealand’s equivalent mechanism, concentrating executive power over regulatory processes. Both initiatives claim efficiency while potentially targeting regulations that protect workers, consumers, and the environment.
The Tikanga Violations: How Neoliberalism Assaults Māori Values
Every principle of tikanga Māori is violated by this Government’s health agenda:
Whanaungatanga (Connection and Relationships): The disestablishment of Te Aka Whai Ora severed institutional relationships between Māori health providers and the health system. Proposed cuts include 131 positions in Māori health services. These eliminations destroy institutional knowledge and connections built over years.
Manaakitanga (Care and Hospitality): Young Māori and Pacific mothers at Middlemore Hospital—which serves Counties Manukau with New Zealand’s largest Māori and Pacific populations—report feeling unwelcome and judged by health system staff. The proposed 140 beds do nothing to address these fundamental failures of culturally competent care.
Kaitiakitanga (Guardianship): The Coalition Government has abandoned guardianship of public health systems, positioning them as costs to be minimized rather than taonga to be nurtured. The Regulatory Standards Bill subordinates many protections to property rights considerations.
Wairuatanga (Spirituality and Life Force): Māori die on average 7-8 years younger than non-Māori. Infant death from SUDI occurs at rates 4.7 times higher for Māori than non-Māori. These disparities represent preventable deaths rooted in systemic inequity. The Coalition’s response? Cut Māori health funding and eliminate Māori health leadership.
Kotahitanga (Unity): True unity requires addressing inequity, not pretending colorblind policies serve all equally. The Regulatory Standards Bill’s principle that “every person is equal before the law” is deployed to dismantle Māori-specific health services and Treaty-based partnerships. This “equality” rhetoric historically justifies treating unequal situations identically, perpetuating systemic harm.
Rangatiratanga (Self-Determination): The destruction of Te Aka Whai Ora was an assault on Māori self-determination in health. By eliminating institutional support for Māori-led health solutions, the Coalition forces communities back into assimilationist models that have demonstrably failed.
Aroha (Compassion): There is no aroha in announcing 140 beds while cutting 1,500 health jobs. No aroha in a Government that received $10.4 million in corporate donations to capture power, then uses that power to inflict suffering on vulnerable communities.
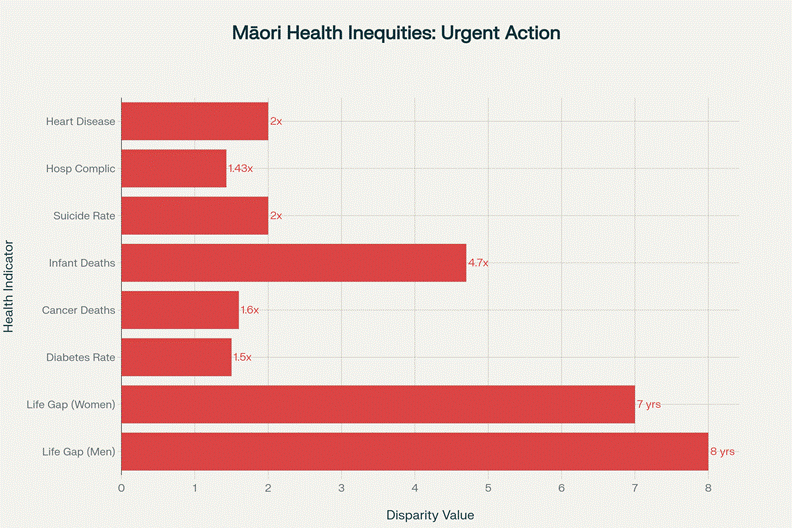
Māori face devastating health disparities including life expectancy 7-8 years shorter, infant death rates 4.7 times higher, costing $1.034 billion annually
The Hidden Connections: Who Benefits From Health System Dismantling
The Donor Class: In 2023 political donations, National received $10.4 million and ACT received $4.3 million. These aren’t disinterested civic contributions. Corporations with financial interests in regulation and service delivery don’t donate to political parties without expecting policy returns.
The Think Tank Network: The New Zealand Initiative has been described as part of international networks advocating libertarian policy approaches. The Initiative’s advocacy has influenced regulatory reform proposals.
The Private Hospital Opportunity: While public hospitals face cuts, Health Minister Simeon Brown directed Health NZ to pursue 10-year outsourcing contracts with private hospitals for elective surgeries. Private sector expansion proceeds while public capacity deteriorates, concentrating profit opportunities.
The Revolving Door: Professor Lester Levy chairs Health NZ, chairs the Health Research Council, and serves as Professor of Digital Health Leadership at Auckland University of Technology—multiple overlapping roles where conflicts of interest require careful management.
The International Coordination: Russell Vought consolidates power in the US Office of Management and Budget while David Seymour pushes the Regulatory Standards Bill in New Zealand—these are variations of coordinated transnational efforts to entrench particular governance approaches.
The Quantified Harm: What 140 Beds Won’t Fix
Māori health disparities are documented and severe:
Life Expectancy: Māori men die 8 years younger, Māori women 7 years younger than non-Māori.
Infant Mortality: Māori babies die from SUDI at 4.7 times the rate of non-Māori babies.
Chronic Disease: Māori are 2.3 times more likely to die from diabetes, cardiovascular disease, stroke, and COPD. Māori are twice as likely to have ischaemic heart disease.
Mental Health: Reported disparities in mental health outcomes affect rangatahi Māori significantly.
Hospital Complications: Māori are 43% more likely to be admitted to hospital due to healthcare complications than non-Māori.
The Coalition’s 140 beds won’t address any of these systemic inequities. They won’t increase Māori health workforce capacity, restore Māori health leadership, fund community health programs, or ensure culturally safe care. They’re infrastructure without equity—which means they’ll primarily benefit populations already served better by the existing system while Māori continue experiencing preventable health disparities.
The Implications: Where This Leads
Short-Term (2025-2026): The proposed 1,500 job cuts proceed, including 131 positions in Māori health and 115 in Pacific health services. Health worker recruitment becomes more difficult. Hospital overcrowding persists. Waiting lists for elective surgery and specialist appointments expand. Emergency departments face continued pressure.
Medium-Term (2026-2030): The 140 beds arrive but face workforce constraints. Private hospital contracts accelerate, extracting profit while public capacity deteriorates. The Regulatory Standards Bill advances regulatory changes that reshape health governance. Māori health outcomes face continued pressure from under-resourcing.
Long-Term (2030+): New Zealand’s health system becomes increasingly fragmented: stronger private care for those who can afford it, deteriorating public care for everyone else. Māori, Pacific peoples, and low-income communities experience worsening health outcomes. Prevention and primary care continue to be under-invested. The foundational principle of universal healthcare access becomes increasingly compromised.
What We Must Do
Name the System: This isn’t incompetence or inevitable fiscal reality—it’s policy choice. Call it what it is: austerity ideology designed to transfer public wealth to private hands while dismantling collective care infrastructure.
Follow the Money: Track political donations. Identify think tank and policy network connections. Make the networks visible so they can’t operate in shadows.
Defend Public Health: Support health workers’ campaigns for adequate staffing and resources. Attend public meetings. Make submissions to select committees. Public pressure can force policy reconsideration—thousands marching in Dunedin created political pressure around hospital plans.
Center Māori Leadership: Demand restoration of Te Aka Whai Ora. Support Māori health providers. Prioritize Māori voices in health policy debates.
Vote Them Out: The 2026 election is coming. Remember who disestablished Māori health authority. Remember who cut health jobs. Remember who prioritized privatization over public health. Vote accordingly, and encourage others to do the same.

The Māori Green Lantern Fighting Misinformation And Disinformation From The Far Right
Simeon Brown’s 140 hospital beds are a con—theatrical crumbs offered while the Coalition government systematically dismantles public health infrastructure, eliminates Māori health leadership, and redirects public wealth toward private profit. These modular wards address less than 3% of New Zealand’s OECD bed shortage, meanwhile proposed cuts eliminate 1,500 health positions including critical roles in Māori and Pacific health services.
A country that lets children sleep on hospital floors, forces patients to wait 12 hours in emergency departments, and allows Māori to die 7-8 years younger than non-Māori while pursuing other policy priorities has revealed its values. But here’s what this Government fears: our collective power exceeds their wealth and institutional capture. Every nurse who demands safe staffing ratios, every community that demands better, every voter who recognizes these policies as harmful, threatens their agenda.
The 140 beds aren’t the solution. We are.
Kia kaha. Kia māia. Kia manawanui.
If this mahi has served you and your whānau have the capacity to support it, koha can be sent to: HTDM: 03-1546-0415173-000. Your tautoko enables continued investigation exposing those who benefit from systems of harm.