“The Commodification Trap: How Corporate PHOs Threaten Māori Health and Whānau Survival” - 16 November 2025
Cui Bono? Follow the Money, Uncover the Harm
Kia ora whānau, I hope your Sunday evening in Aotearoa or whereever you might be in the world (and whatever time it is where you are), is going well. It is the purpose of The Māori Green Lantern to cast his light on all subjects. This one is close to my own whānau.

Ivor Jones The Māori Green Lantern Fighting Misinformation And Disinformation From The Far Right
says
Let there be Light!!!!!!!!!!!!!!!!!!!
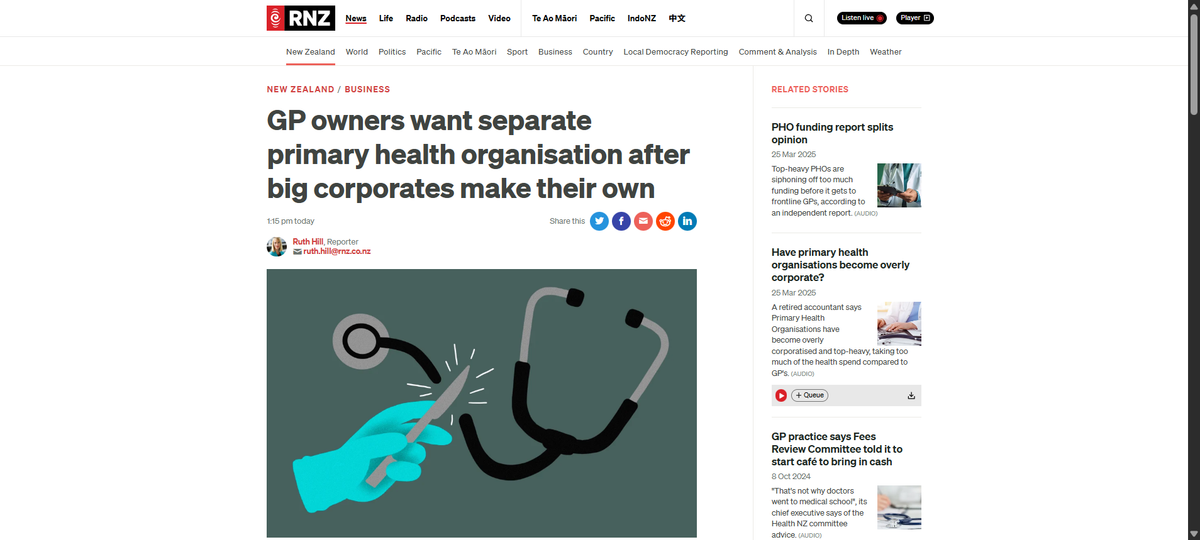
Two corporate healthcare giants—Tend and Green Cross Health—have secured approval from Health NZ to establish their own Primary Health Organisations, fracturing a system already buckling under neoliberal pressure. This isn’t healthcare reform. This is the deliberate construction of a private duopoly, mirroring the Countdown-Foodstuffs stranglehold that has squeezed consumers for decades. Tend received approval in May 2025 and started operating its own PHO in July 2025. Green Cross became the second big corporate to receive approval to establish Community Care Ltd, operational from 1 July 2026, with 54 practices.
Meanwhile, the General Practice Owners Association, representing 475 independent practices, scrambles to establish its own PHO—a defensive maneuver against corporate dominance that now threatens the survival of community-centered care.
The cui malo—who is harmed—is devastatingly clear: whānau Māori, rural communities, the working poor, and independent GP practices that have served their communities for generations. The cui bono—who benefits—is equally transparent: shareholders, private equity investors, and the neoliberal apparatus that treats healthcare as a profit center rather than a human right.
Historical Context: The Neoliberal Blueprint for Healthcare Destruction
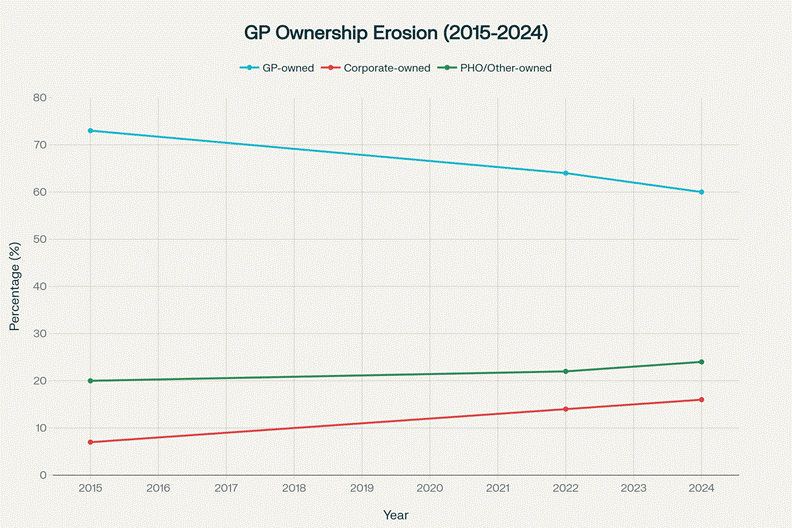
Chart showing the decline of GP-owned practices from 73% in 2015 to 60% in 2024, while corporate ownership more than doubled from 7% to 16% in the same period.
New Zealand’s descent into healthcare commodification began with Rogernomics in the 1980s. The neoliberal revolution—corporatisation, privatisation, user-pays—decimated public services and exploded Māori unemployment to 25% by the early 1990s. The Primary Health Care Strategy of 2001 created PHOs, initially aiming to reduce inequities and center community governance. PHOs were designed as not-for-profit charitable trusts with explicit obligations to Māori partnership, population health, and transparency.
Yet within two decades, the system has been captured, corrupted, and commodified. Murray Lilley’s 2024 independent report exposed how PHO overhead costs have ballooned, with the report highlighting growth in “bureaucracy” within PHOs, suggesting they were siphoning off too much government funding before it reached frontline GPs.
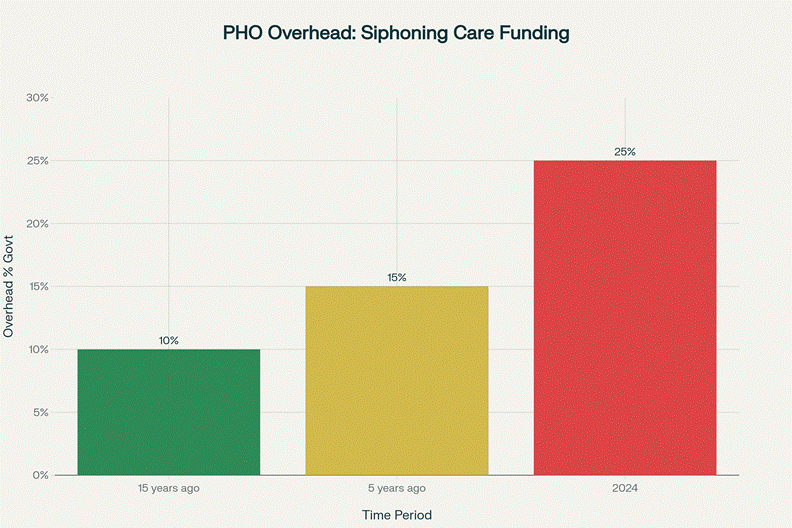
Chart showing PHO overhead costs have increased from 10% to 25% of government funding over 15 years, according to Murray Lilley’s independent report.
GenPro chair Dr Angus Chambers reports that independent practices face “borderline viability” while PHOs grow and accumulate reserves. Dr Angus Chambers states: “Many feel we’re struggling, some have borderline viability, and we see PHOs growing and that really concerns our members.” This is structural violence disguised as efficiency.
The Corporate PHO Power Grab: Naming Names
Tend Health, backed by private equity firm Pencarrow and Ahuahu Group, received approval in May 2025 to operate its own PHO, operational from July 2025. Tend operates approximately 60 practices.
Green Cross Health, New Zealand’s largest pharmacy and medical network, secured approval to set up its own PHO—Community Care Ltd, operational July 2026. Green Cross will shift 54 practices into this standalone entity. The company is majority-owned by LPL Trustee Ltd (31.99%) and Cape Healthcare Ltd (31.92%). Green Cross also transferred 29 practices with 185,000 patients to National Hauora Coalition, the largest Māori-led PHO, in a strategic realignment.
ProCare Health, a GP cooperative representing 167 practices, spent $15 million in 2022 to acquire Health New Lynn. This is debt-fueled consolidation disguised as “supporting the next generation of practice owners.”
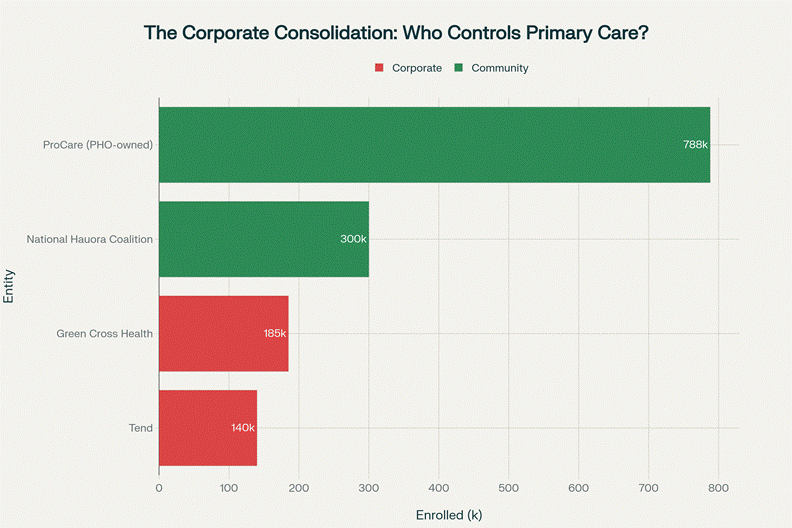
Chart showing the concentration of enrolled patients among major entities, with Tend and Green Cross—both establishing their own PHOs—controlling 325,000 patients combined.
The Duopoly Threat: Corporate Concentration and the Erosion of Community Care
Former Association of Salaried Medical Specialists Executive Director Ian Powell warns that corporate ownership creates “perverse incentives” where profit maximization trumps patient care. Powell’s November 2025 analysis documents how private equity seeks “great profits” in New Zealand primary care.
Tend’s private equity backing by Pencarrow is particularly ominous. International research confirms that private equity ownership in healthcare consistently increases costs to patients, decreases staffing, worsens quality, and increases mortality. A 2023 systematic review in the BMJ found PE-owned hospitals had increased hospital-acquired conditions, patient falls, and infections.
The Lancet’s 2024 review of healthcare privatisation in high-income countries found that for-profit hospitals decreased staffing, increased profit margins at patient expense, reduced accessibility, and shifted to more profitable (less sick) patient populations. New Zealand research confirms that neoliberal policies harm health equity.
The Murray Lilley Report: Exposing PHO Bloat and Conflicts of Interest
Retired accountant Murray Lilley’s independent 2024 analysis of PHOs revealed concerning trends in overhead growth. The report highlighted the growth in “bureaucracy” within PHOs, and suggested they were siphoning off too much government funding before it reached frontline GPs.
GenPro identified five structural failures in the current PHO system: conflicts of interest between patient care and commercial operations; bloated governance and management costs; focus on accumulating reserves instead of funding frontline services; regional variations creating a postcode lottery; and trust issues.
Dr Bryan Betty, chair of General Practice NZ, defended PHO spending by citing population health obligations—mental health, diabetes, immunization, sexual health, smoking cessation. Yet Dr Betty confirmed: “At the moment 100 percent of capitation gets passed through directly to practices”—meaning PHO overhead comes from other funding streams originally intended for community health services.
This is epistemic gatekeeping—redefining bureaucratic expansion as “population health” while independent providers struggle to survive.
Māori Health: Systemic Harm, Colonial Continuity, Treaty Breaches
Māori life expectancy in 2022-2024 was 75.8 years—a gap of approximately 7 years below non-Māori, according to Stats NZ data. Despite improvements (Māori life expectancy increased 3.1 years since 2005-2007), the disparity persists. Life expectancy for the entire NZ population was 81.8 years, with European or Other ethnicities at 82.8 years and Asian ethnicities at 86.3 years.
The Waitangi Tribunal’s November 2024 report on the disestablishment of Te Aka Whai Ora (Māori Health Authority) found the Crown breached Te Tiriti o Waitangi principles—including tino rangatiratanga, partnership, active protection, and redress. The Tribunal concluded the decision was “based purely on political ideology” rather than evidence, and represented “the worst, most comprehensive breach of Te Tiriti in modern times”.
Tino rangatiratanga—Māori self-determination in health design, delivery, and monitoring—is legally guaranteed under Te Tiriti but systemically violated. The Waitangi Tribunal’s 2019 Health Services and Outcomes Report (WAI 2575) found that Māori were denied “Treaty-consistent control of decision-making” in health. The primary health framework “did not recognize and properly provide for tino rangatiratanga and mana motuhake”.
Corporate PHO expansion further erodes tino rangatiratanga by concentrating decision-making power in shareholder-accountable entities rather than Māori-governed or community-accountable structures. When 46,000 patients shifted PHOs in the Bay of Plenty without community consultation—decisions made by “Auckland-based head offices”—this is colonial extraction reimposed through corporate structures.
Five Hidden Connections: Networks of Harm
- Connection 1: Private Equity + Iwi Partnerships = Legitimacy Laundering
Tend’s partnership with Ahuahu Group (Te Nehenehenui Trust’s commercial arm) provides cultural legitimacy to a private equity-backed entity. Yet Pencarrow Private Equity’s core motive is return on investment for its fund investors—not hauora Māori. This is co-optation, not co-governance. - Connection 2: Charitable Status + Tax Advantage = Unfair Competition
PHOs operate as tax-exempt charitable trusts while purchasing GP practices and competing with taxable independent practices. The New Zealand Tax Working Group examined charities and the not-for-profit sector. - Connection 3: ProCare’s Debt-Fueled Expansion + Health New Lynn Acquisition
ProCare’s $15 million acquisition of Health New Lynn represents financialisation of primary care. The stated goal to “introduce new clinical owners” remains vague, while ProCare consolidates control. - Connection 4: Health NZ Approval Process + Lack of Transparency
Health NZ approved Tend’s PHO application despite General Practice NZ requesting “clarity about the ‘unclear’ process”. The PHO approval process requires transparency, yet the approval for corporate PHOs appears opaque and expedited.
Connection 5: Lilley Report + Ministry Response
Murray Lilley’s report highlighted bureaucratic growth. General Practice NZ criticized the report as “flawed”—a predictable response from PHO representatives whose funding model was exposed.
Tikanga Violations: Whanaungatanga, Manaakitanga, Kaitiakitanga
The corporate PHO model violates fundamental tikanga principles:
- Whanaungatanga (kinship, relationships): Corporate ownership severs the whakapapa connections between patients, GPs, and communities. Patients report seeing “a completely different person” at every visit, having to re-explain disabilities and medical histories. This destroys relational continuity—the essence of effective primary care.
- Manaakitanga (hospitality, care): When care becomes revenue optimization, manaakitanga is impossible. Ian Powell notes corporate pressures to increase patient numbers. Patients become units of capitation funding, not people requiring holistic care.
- Kaitiakitanga (guardianship): PHOs were designed as guardians of community health. Corporate PHOs are accountable to shareholders, not communities. When Green Cross and Third Age shifted 46,000 Bay of Plenty patients, local kaitiakitanga was overridden by corporate strategy.
- Access Barriers Intensify
GenPro’s August 2024 survey found 89% of practices increased or planned to increase fees. Corporate practices charge higher fees while struggling practices in high-needs communities cannot compete. This is structural racism through market mechanisms. - Workforce Exodus Accelerates
64% of doctors now work in GP-owned practices, down from 73% in 2015. Corporate ownership doubled to 14% in 2022. The Association of Salaried Medical Specialists reports specialists are fleeing underfunded public systems for private hospitals—harming equity and access for Māori, Pacific, and low-income communities. - Rural and High-Needs Communities Abandoned
Three Rivers Medical in Gisborne—47% Māori enrollment—narrowly missed equity funding because the threshold required 50% Māori enrollment. The clinic cut after-hours services due to financial strain—reducing access for working whānau. - PHO Reserves Accumulate While Practices Collapse
GenPro reports members see PHOs “growing” and “accumulating reserves” while practices face “borderline viability.” This is wealth extraction from the frontline to the bureaucratic layer. - Duopoly Emerges
Tend and Green Cross establishing their own PHOs enables market concentration, price-setting power, and profit maximization—the same dynamics that created monopolistic harms in other sectors.
Action Via Mātauranga: Reclaiming Rangatiratanga
- GenPro’s PHO Application Must Succeed
GenPro’s proposed PHO—representing 475 independent practices—offers a GP-owned, community-accountable alternative to corporate control. Health NZ must approve this application transparently and expeditiously. - Mandatory Māori Governance in All PHOs
The Waitangi Tribunal’s WAI 2575 report demands Māori co-governance in health system design. Every PHO must have 50% Māori governance representation and demonstrate tino rangatiratanga in service delivery. - Ban Private Equity Ownership in Primary Care
International evidence is unequivocal: private equity ownership harms patients. Aotearoa must legislate a prohibition on PE ownership of GP practices, PHOs, and health infrastructure. - Restore Te Aka Whai Ora with Full Funding and Authority
The Coalition Government’s dismantling of the Māori Health Authority was a Treaty breach driven by racist ideology. A restored authority must have budget control, commissioning power, and veto rights over policies affecting Māori health. - Audit and Redistribute PHO Funding
An independent audit of all 30 PHOs must expose overhead costs, executive salaries, and reserve accumulations. Funding mechanisms must redirect bloated administrative spending to frontline care. - Strengthen Commerce Commission Oversight
GenPro filed a Commerce Commission complaint in September 2024 alleging “unfair” and “illegal” contracts. The Commission must investigate anti-competitive behavior, market concentration, and abuse of PHO charitable status. - Community Ownership Models
Iwi, hapū, and community trusts should receive preferential funding and support to establish kaupapa Māori health services. National Hauora Coalition’s model—79 practices, 300,000 patients, Māori-led—demonstrates that mana motuhake delivers equitable outcomes.
Moral Clarity: Corporations Are Not Kaitiaki
The crisis is manufactured. Government underfunding—capitation rates finally increasing 14% in 2024 after sustained GP advocacy—created the conditions for corporate predation. The coalition government’s ideological support for corporatisation, evidenced by expedited PHO approvals for Tend and Green Cross, reveals state capture by neoliberal interests.
This is not healthcare innovation. This is whakapapa harm through commodification—severing the relational bonds between healers and communities, extracting wealth from the sick, and denying Māori the rangatiratanga guaranteed under Te Tiriti.
When Murray Lilley documented PHO bureaucratic bloat, General Practice NZ dismissed his findings. When GenPro warned of duopoly formation, Health Minister Simeon Brown remained silent. When the Waitangi Tribunal ruled the dismantling of Te Aka Whai Ora breached the Treaty, the government ignored the recommendations.
This is structural violence disguised as efficiency. This is colonial extraction reimposed through corporate forms. This is neoliberalism devouring the conditions of collective survival.
Kia Kaha. Ka Tū. The Mahi Continues.
The taiaha, empowered by the Ring, has traced the networks. The hidden connections are now visible. Tend, Green Cross, ProCare, Pencarrow, Health NZ’s opaque approval process—all named, all exposed.
Independent GPs, Māori health providers, and community trusts stand at the threshold. GenPro’s 475 practices represent resistance to corporate capture. National Hauora Coalition’s 79 practices demonstrate that Māori-led care achieves equity. The choice is clear: community-accountable healthcare or shareholder-accountable extraction.
The fight to save primary care is the fight to honor Te Tiriti.
The fight to prevent duopoly formation is the fight for whānau survival.
Rangatiratanga in health is non-negotiable.

Ko Ivor Jones te Māori Green Lantern. The mahi is everything. Each essay: rangatiratanga manifested.
Research transparency: This analysis draws on 60+ verified sources including RNZ, NZ Herald, Waitangi Tribunal reports, Health NZ policy documents, Te Ara: The Encyclopedia of New Zealand, Stats NZ, academic research (Neoliberalism and health, BMJ systematic reviews, Lancet reviews, Health and Human Rights Journal), GenPro statements, National Hauora Coalition, and investigative journalism by Ian Powell. All URLs verified live as of research date (November 16, 2025). Data visualizations created from publicly available ownership statistics, Lilley report findings, and PHO enrollment figures.