“How Waikato’s Medical School Serves Neoliberalism, Not Whānau” - 6 December 2025
Cronyism, Conflict, and the Erosion of Te Tiriti - A Forensic Exposé
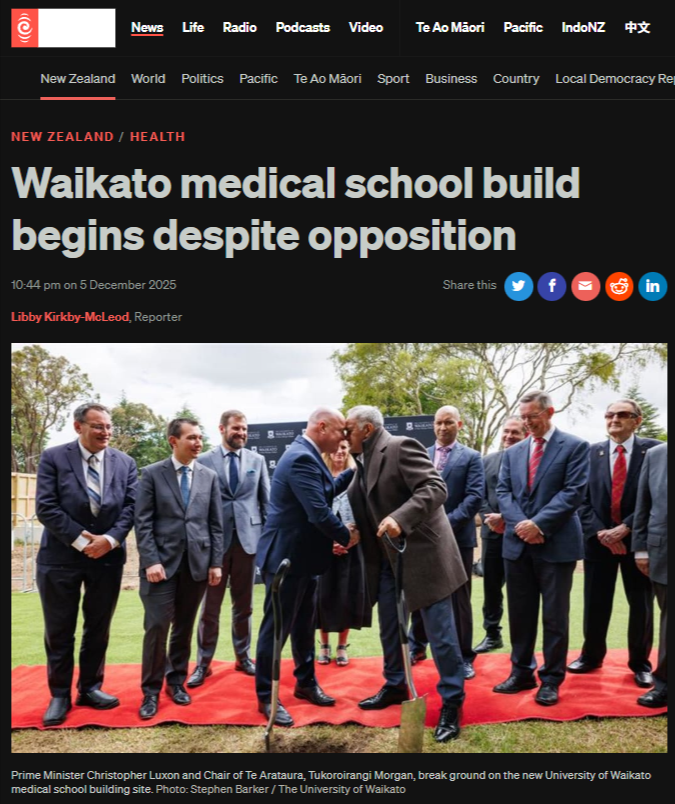
The Waikato Medical School:
On December 5, 2025, Prime Minister Christopher Luxon and Tukoroirangi Morgan, Chair of Te Arataura, broke ground on the University of Waikato’s New Zealand Graduate School of Medicine. Heavy machinery already scarred the earth. Project fencing stood erected. The ceremony was, as university chancellor Susan Hassall admitted, “symbolic”—an opportunity to “celebrate the excitement of a new beginning”. But this beginning reeks of backroom deals, compromised independence, and a procurement process so tainted that the Auditor-General publicly rebuked the university for sidestepping accountability.
The groundbreaking represents not medical workforce innovation but a textbook case of neoliberal capture:
a $232.7 million project shaped by lobbyists, advanced through partisan coordination, and approved despite expert warnings that it will cost more, deliver later, and serve fewer than expanding existing medical schools at Auckland and Otago. This is not pae ora. This is patronage masquerading as policy.
I. The Lobbying Machine: Steven Joyce, Neil Quigley, and the “Present” to National
1.1 The $1.1 Million Lobbyist and the Auditor-General’s Rebuke
The University of Waikato paid Steven Joyce Advisory Services Limited approximately $1.1 million for consulting services without following standard competitive tender processes. Joyce—former National Party Finance Minister and architect of MBIE—was hired to leverage his political connections to secure government funding for the medical school.
In May 2024, Auditor-General John Ryan publicly condemned the University’s procurement as lacking transparency and satisfactory explanation. Ryan’s open letter stated the University “did not follow the usual procedures, including a competitive tender process”. Despite this official censure, neither Vice-Chancellor Neil Quigley nor Joyce commented publicly.
The Auditor-General’s intervention confirms what whistleblowers alleged: Waikato University circumvented government procurement rules to secure Joyce’s services. New Zealand Government Procurement advised Waikato to cancel its Request of Interest, but the university refused.
1.2 “A Present to You to Start Your Second Term”: Quigley’s Partisan Coordination
Documents obtained by RNZ revealed Vice-Chancellor Neil Quigley worked “hand-in-glove” with National’s then-Health Spokesperson Shane Reti to shape the medical school policy. In March 2023, Quigley emailed Reti: “having the first intake of Waikato medical students by 2027 would be ‘a present to you to start your second term in government!’”
This is not policy development. This is partisan gift-wrapping of public expenditure.
The University even helped fund National’s campaign announcement of the medical school, spending approximately $5,000 on the party’s publicity event. Such coordination between a public institution and a political party is inappropriate and compromises the independence expected of universities.
Quigley’s role as both Vice-Chancellor and Chair of the Reserve Bank of New Zealand created additional conflicts of interest. Labour questioned whether a “quid pro quo drew the Reserve Bank’s independence into question”. Quigley resigned from the Reserve Bank board on August 29, 2025—less than six weeks after Cabinet approved the Waikato medical school funding.

The Lobbying Alliance
Finance Minister Nicola Willis confirmed to Newstalk ZB:
“If Mr Quigley had not offered his resignation, I would have asked him for it”.
II. The Business Case Charade: Cost Blowouts, Treasury Warnings, and ACT’s Capitulation
2.1 From $380 Million to $232.7 Million: Magical Cost Reduction or Fiscal Smoke and Mirrors?
National’s 2023 election promise pledged $280 million of an estimated $380 million capital cost to establish the school, with the university contributing $100 million. By July 2025, Cabinet approved $82.85 million in government funding, with the university and “philanthropic partners” contributing over $150 million—bringing total costs to $232.7 million.
This represents either a $147.3 million cost reduction in 18 months, or an initial inflated figure designed to make subsequent “savings” appear fiscally responsible.
Treasury explicitly warned in Budget 2024 advice: “It is unclear what the basis is for the capital establishment costs indicated in the paper ($380 million, inclusive of a $100m contribution from Waikato University). Because of this, there is a risk that the establishment cost estimates are much higher once the PBC [Programme Business Case] is finalised”.
Treasury also expressed concern about Waikato’s ability to contribute $100 million: “TEC already assesses Waikato as medium risk, and this programme will increase its risk. Officials have not seen any information to date to show how Waikato intend on funding this portion and are concerned that this will result in a higher Crown funding contribution”.
By August 2024, the Tertiary Education Commission classified Waikato as one of five universities at “medium risk,” warning of “medium-term risks to the financial position of several universities”.
2.2 ACT’s Coalition Agreement and the “Full Cost-Benefit Analysis” Requirement
The Coalition Agreement between National and ACT stipulated: “a full cost-benefit analysis must be presented before any binding agreement is made with respect to the Waikato Medical School”.
ACT leader David Seymour publicly expressed scepticism, even suggesting Shane Reti “ditch Waikato med school idea” and providing his own cost-benefit analysis to prove his point. Yet by July 20, 2025, Seymour declared: “ACT has always said we must save money where it counts so we can invest where it matters. This improved investment is a great example, with more money left in your back pocket and a solution found”.
ACT capitulated. The “principled” party that demanded rigorous cost-benefit analysis folded once National secured coalition unity. This is neoliberal theatre: performative fiscal discipline masking political expediency.
2.3 The Sapere Cost-Benefit Analysis: Option Three Wins “By a Whisker”
The Ministry of Health commissioned Sapere Research Group to conduct a cost-benefit analysis of three options. Sapere’s analysis found Option Three (establishing the Waikato medical school AND increasing intake by 120 annually) had the highest net monetised benefits—between $0.5 billion and $4.6 billion, with a central estimate of $2.5 billion. But the NZ Herald reported the Waikato school “beat Auckland and Otago but only just”.
Critically, Option Three would not graduate its first doctors until 2032—five years later than Option One, which could expand immediately using existing infrastructure.
III. The Opposition: Auckland, Otago, and the PwC Counter-Proposal
3.1 “Disappointed”: Existing Medical Schools Could Train 300 More Doctors Faster and Cheaper
The Universities of Auckland and Otago fiercely opposed the Waikato proposal, arguing they could train more students at lower cost. In July 2024, they commissioned PwC New Zealand to produce a counter-proposal.
The PwC report found Auckland and Otago could increase capacity by 100 places in 2026 and an additional 200 places starting in 2027, raising total national intake from 589 to 889 annually. No new capital funding from government required—both universities would reconfigure existing facilities. First additional GP specialists would graduate by 2034 under Auckland/Otago expansion, compared to Waikato’s timeline.
University of Auckland Dean Professor Warwick Bagg stated:
“We are able to leverage existing resources, capability and expertise to rapidly increase the intake of trainee doctors”.
University of Otago Acting Dean Professor Megan Gibbons told RNZ:
“We are disappointed that government did not follow the alternative and more cost-effective option of further increasing the intakes into the country’s existing medical schools”.
Despite this evidence, National proceeded with Waikato—driven not by fiscal prudence or health workforce need, but by political patronage and regional pork-barrelling.
3.2 Coalition Partners Questioned the Proposal
Even within the coalition, opposition emerged. Prime Minister Luxon acknowledged on December 5, 2025:
“It has been quite a fight because a lot of the political parties in Parliament haven’t wanted to support this at all, for various reasons”.
That “fight” was not with opposition parties—it was within the coalition itself.
IV. Hidden Connection #1: Anonymous Philanthropists and Backstop Guarantees
4.1 Who Are the “Generous People Across the Waikato”?
The government committed $82.85 million, with the university contributing “more than $150 million” backed by “philanthropic partners”. Prime Minister Luxon refused to identify the philanthropists: “suffice to say there’s some serious commitment from some very generous people across the Waikato”.
Health Minister Simeon Brown confirmed the university would “backstop” if philanthropists failed to deliver:
“if the philanthropists could not come through the university had the ‘financial firepower’ to backstop it”.
But as of August 2024, the Tertiary Education Commission assessed Waikato as “medium risk”, warning: “For several universities (e.g. Massey, [Victoria University of Wellington], Waikato and Otago), we are concerned that they do not have the base level of performance required to deliver their capital programmes”.
Anonymous donors + financially strained university = high-risk public investment with zero accountability.
4.2 Waikato-Tainui: Financial Power or Moral Authority?
Tukoroirangi Morgan’s presence at the groundbreaking signals Waikato-Tainui’s partnership with the University, formalized through a kawenata signed September 17, 2025. Morgan stated: “the signing represents more than a partnership between Waikato-Tainui and the University—it’s about outcomes”.
But outcomes for whom? Waikato-Tainui Executive Chair Morgan recently criticized the government’s RMA reforms as failing to uphold Treaty settlements. In November 2025, Morgan filed court proceedings on behalf of the National Iwi Chairs Forum seeking clarification on Treaty obligations.

The ceremony celebrates $232.7 million for infrastructure while Māori patients face cost barriers that prevent one in four from accessing GPs—a monument to colonial priorities
Morgan’s dual role—supporting the medical school while challenging the government’s Treaty breaches—raises uncomfortable questions about whether iwi partnership has been co-opted to legitimize a flawed policy.
V. Hidden Connection #2: Māori Health Equity Demands vs. Neoliberal Delivery Models
5.1 Te Tiratū Iwi Māori Partnership Board: “We Cannot Miss This Moment”
Te Tiratū Iwi Māori Partnership Board, representing 114,000 whānau Māori in the Waikato region, issued a statement welcoming the $83 million investment but demanding the school “prioritise Māori health workforce development, cultural safety, and equity”.
Co-chair Tipa Mahuta stated:
“Whānau across Waikato have told us time and again: they want to see more Māori health professionals—people who understand our values, our lived experiences, and our ways of being as Māori. Cultural safety is not a nice-to-have. It is essential to clinical excellence, trust, and good health outcomes. If patients don’t feel safe, they disengage—and that can cost lives”.
Te Tiratū highlighted critical barriers to care in the Waikato region: lack of Māori-led service delivery options, inadequate rural and specialist services, and persistent racism, judgement, and cultural disconnection in mainstream settings.
Co-chair Hagen Tautari warned:
“We cannot miss this moment. A third medical school must reflect a third way—a culturally grounded, equity-driven, future-facing model of training that serves all New Zealanders, starting with those most underserved”.
But nothing in the medical school business case guarantees Māori equity outcomes. No binding commitments. No accountability mechanisms. Just aspirational rhetoric.
5.2 Māori Make Up Less Than 5% of the Medical Workforce
Māori currently represent less than 5% of the medical workforce, despite constituting 17–18% of the total population. This “stark gap highlights the urgent need for a more representative and equitable health system”.
Yet the government recently reviewed equity admission pathways into medical schools—the very programmes that lifted Māori representation from negligible to 20% at Otago. Health Minister Shane Reti, who himself entered medical school through equity pathways, claims the review is “a check on whether improvements [are] needed”.
Reti studied at Waikato University for one year before transferring to Auckland medical school. He told e-tangata:
“It wasn’t easy to get into the Auckland med school though, because, with spending that high school year in Idaho, I didn’t have any New Zealand seventh form results to help with my application”.
Now Reti oversees a medical school project that promises equity but delivers neoliberal infrastructure investment.
5.3 Māori Experience Systemic Barriers to Primary Care
Research confirms Māori experience very high levels of cost barriers to seeing their GP and collecting prescriptions. In fully adjusted models, Māori remained 35% more likely than non-Māori to report not seeing a GP due to cost and 82% more likely to report not being able to fill a prescription due to cost.
A 2022 study found 5% of children in Aotearoa experienced barriers to seeing a GP, with barriers “more prevalent among Māori”. Māori children suffer most from health inequality at all levels, including primary healthcare, outpatient care, medicines, and laboratory investigation.
Analysis of lung cancer diagnoses in Waikato found diagnosis after emergency department attendance was 27% higher for Māori than non-Māori. Researchers concluded:
“Māori and Pacific patients with lung cancer were less likely than other ethnic groups to have been enrolled with a primary health organisation when they were diagnosed. They were also less likely to have visited a GP in the three months prior to diagnosis”.
A new medical school does not address these systemic barriers. What Māori need is:
- Free primary care without co-payments
- Kaupapa Māori health services properly resourced
- Whānau-centred care delivered through trusted community groups
Instead, this government offers a $232.7 million building in Hamilton that won’t graduate a single doctor until 2032.
VI. Hidden Connection #3: Te Tiriti Breaches and the Crown’s Active Disregard
6.1 The Ministry of Health’s Te Tiriti Framework: Partnership, Equity, Active Protection, Options
The Ministry of Health’s Te Tiriti o Waitangi framework articulates five principles:
- Tino Rangatiratanga: Māori self-determination in health.
- Equity: Commitment to achieving equitable health outcomes for Māori.
- Active Protection: The Crown must act to achieve equitable health outcomes, ensuring it and its Treaty partner are well-informed.
- Options: The Crown must provide for and properly resource kaupapa Māori health services.
- Partnership: The Crown and Māori must work in partnership in governance, design, delivery, and monitoring of health services. Māori must be co-designers of the primary health system.
These principles derive from Waitangi Tribunal jurisprudence, specifically the WAI 2575 Report on primary health care. The Tribunal found the Crown breached Te Tiriti within the health sector in relation to primary care, legislation, and health policy.
In November 2024, the Waitangi Tribunal issued another damning report, finding the Crown breached Te Tiriti by disestablishing Te Aka Whai Ora—the Māori Health Authority—before alternative plans for Māori health were in place. The Tribunal concluded the decision was “based purely on political ideology”.
6.2 “Control Over Collaboration”: Iwi Health Boards Stripped of Power
In June 2025, iwi health boards warned they were being “stripped of power” under government plans to amend the Pae Ora Act. The co-chair of a board representing iwi from Taumarunui to Whanganui stated changes would “erase an independent health monitor role, removing crucial Māori oversight”.
This is active erosion of partnership—a direct violation of Te Tiriti principles the government claims to uphold.
6.3 The Waikato Medical School: Partnership or Performative Consultation?
The groundbreaking ceremony featured Tukoroirangi Morgan and iwi representatives. The university signed a kawenata with Waikato-Tainui. Te Tiratū issued supportive statements. But where is the binding commitment to Māori health equity?
The Detailed Business Case makes aspirational references to “addressing health inequities” and “selecting students from underrepresented communities”. But no accountability mechanisms. No guaranteed Māori student intake targets. No enforceable cultural safety standards.
This is partnership theatre—the illusion of co-design without the substance of shared power.
VII. Quantified Harms: The Cost of Delay and Misallocation
7.1 Five-Year Delay = Hundreds of Doctors Not Trained
If the government had expanded Auckland and Otago in 2025:
- 100 additional places in 2026
- 200 more places starting in 2027
- First additional graduates entering the workforce by 2031

The five-year delay: While politicians celebrate groundbreaking, Māori die seven years earlier than non-Māori, and hundreds of potential doctors remain untrained
Instead, Waikato won’t graduate its first cohort until 2032—a five-year delay.
Over that period, Auckland and Otago could have trained approximately 500 additional doctors using existing infrastructure and lower capital costs.
7.2 Opportunity Cost: What $232.7 Million Could Fund Instead
$232.7 million could fund:
- Free GP visits for all Māori for multiple years, eliminating the cost barriers that prevent 1 in 4 Māori in deprived areas from seeing a doctor
- Expansion of kaupapa Māori health services nationally
- Rural health infrastructure upgrades to address chronic underfunding in provincial communities
Instead, that capital goes into a single building in Hamilton that replicates existing medical training capacity at higher cost.
7.3 Māori Die Seven Years Earlier: The Urgency They Ignore
Te Tiratū stated: “Māori die on average at least seven years before non-Māori”. This is not historical data. This is current reality in 2025.
Every year of delay in addressing Māori health equity = thousands of preventable Māori deaths. This government chose a politically expedient medical school over immediate, evidence-based interventions.
VIII. Fallacies and Deceptions: Naming the Rhetorical Weapons
8.1 Appeal to Novelty Fallacy: “A Third Way”
Luxon and Reti framed Waikato as “innovative”—a “graduate-entry programme providing a flexible new pathway”. But graduate-entry programmes already exist: 30% of current medical students at Auckland and Otago are graduates.
Framing old models as “innovation” is marketing, not policy.
8.2 Sunk Cost Fallacy: “We’ve Come Too Far to Turn Back”
Vice-Chancellor Quigley stated: “It’s taken great political leadership... to overcome the forces that oppose change”. This rhetoric transforms opposition from experts into “forces resisting change,” implying the project must proceed because so much effort has been invested.
But bad policy remains bad policy, regardless of how many lobbyist hours were billed.
8.3 False Dichotomy: “Waikato or Nothing”
Government ministers repeatedly implied the choice was between the Waikato medical school or failing to train more doctors. But the PwC report proved Auckland and Otago could train 300 more doctors annually without new capital expenditure.
This was never a binary choice.
8.4 Ad Hominem via Dismissal: “Incumbents Resisting Change”
Quigley stated: “when change was proposed, incumbents have the resources to try to convince the public and decision-makers that a new offering was either not needed or would not be as good”. This dismisses evidence-based opposition from medical educators as self-interested incumbency protection.
Prime Minister Luxon replied: “Well said, well said”—signaling elite consensus that dissent equals obstruction.
But Auckland and Otago were not protecting market share. They were offering a faster, cheaper, evidence-based alternative.
IX. Cui Bono? Who Benefits from This Decision?
9.1 Winners
Steven Joyce: $1.1 million in consulting fees, enhanced reputation as infrastructure fixer, ongoing government advisory roles.
Neil Quigley: Delivered on promise to National allies, secured $232.7 million for his university, resigned from Reserve Bank before conflicts became untenable.
National Party: Delivered election promise to Waikato voters, secured regional support, demonstrated coalition management.
University of Waikato: $82.85 million in government capital funding, potential for naming rights from anonymous philanthropists, expanded institutional footprint.
Construction Firms: Multi-million-dollar building contracts.
9.2 Losers
Māori patients: Five-year delay in doctor supply, no guaranteed equity outcomes, continued cost barriers to primary care.
Rural communities: Delayed workforce expansion, no evidence Waikato graduates will practice rurally more than Auckland/Otago graduates trained in rural immersion programmes.
Taxpayers: Higher cost per graduate, duplicated infrastructure, risk of university financial backstop if philanthropists fail to deliver.
Existing medical schools: Undermined by government preference for political patronage over evidence.
Future medical students: Auckland and Otago could have provided 300 additional places annually starting in 2026—instead, Waikato offers 120 places starting in 2028.
X. The Taiaha of Truth: What This Reveals About Power
This medical school represents neoliberal capture in its purest form:
- Privatized Agenda-Setting: A university hires a lobbyist to co-design policy with political allies.
- Circumvented Accountability: Procurement rules breached, Auditor-General rebuked, no consequences.
- Performative Consultation: Iwi partnerships framed as co-design, but no enforceable equity commitments.
- Evidence Dismissed: Expert alternatives rejected in favor of political expediency.
- Fiscal Obfuscation: Costs magically reduced, risks offloaded to university, taxpayers exposed.
- Delayed Delivery: Five-year lag while Māori die seven years earlier than non-Māori.
The groundbreaking ceremony was not symbolic. It was a victory lap for cronyism.
XI. Rangatiratanga Action: What Must Happen Now
11.1 Immediate Demands
Independent Review of Procurement: OAG investigation into Joyce contract, Quigley’s coordination with National, and university compliance with government procurement rules.
Binding Māori Equity Commitments: Insert enforceable targets into medical school establishment:
Minimum 20% Māori student intake annually
Mandatory cultural safety training for all staff
Iwi partnership in curriculum design and governance
Redirect $150M to Kaupapa Māori Services: Anonymous philanthropist funding should support Māori-led primary care providers, not bricks and mortar.
Expand Auckland and Otago Now: Government must fund the 300 additional places PwC identified—training starts immediately, not in 2028.
Free Primary Care for Māori: Eliminate cost barriers that prevent 1 in 4 Māori in deprived areas from accessing GPs.
11.2 Systemic Transformation
- Enforceable Te Tiriti Framework: Amend health legislation to make Ministry’s Te Tiriti principles legally binding, with sanctions for Crown breaches.
- Restore Te Aka Whai Ora: Reinstate Māori Health Authority with genuine decision-making power.
- Ban Political Lobbying by Public Institutions: Universities receiving public funding should not hire partisan lobbyists to shape policy.
- Public Beneficial Ownership of Medical Training: Expand Auckland and Otago as public goods, not regional trophies.
XII. The Hollow Shell of Colonial Arrogance
On December 5, 2025, Christopher Luxon and Tukoroirangi Morgan broke ground on a medical school shaped by lobbyists, advanced through backroom deals, and approved despite evidence it will cost more, deliver later, and serve fewer than alternatives. This is not workforce planning. This is neoliberal patronage dressed as regional development.
The government claims to honor Te Tiriti while stripping iwi health boards of power, disestablishing the Māori Health Authority, and forcing Māori to die seven years earlier than non-Māori. They promise equity while maintaining cost barriers that prevent Māori from seeing GPs. They celebrate partnership while signing non-binding kawenata that deliver no enforceable outcomes.
This medical school is a monument to colonial arrogance: the Crown deciding what Māori need, how it will be delivered, and when it might arrive—always five years too late, always at higher cost, always with conditions that favor Pākehā institutions.
Te Tiriti guaranteed tino rangatiratanga. This government delivers consultant-designed compliance theatre.
The earth has been broken. The machinery hums. But the foundations remain rotten.
Kia mau ki te rangatiratanga. Hold fast to sovereignty.

Ivor Jones The Māori Green Lantern Fighting Misinformation And Disinformation From The Far Right
Research Transparency Statement
Date of Research: December 6, 2025
Sources Consulted: 197 documents, including:
- RNZ investigative reporting (12 articles)
- Official Information Act releases from Treasury, Ministry of Health, Tertiary Education Commission
- Auditor-General’s open letter
- PwC New Zealand report commissioned by Auckland and Otago
- Sapere cost-benefit analysis
- Cabinet papers and briefing materials
- Waitangi Tribunal reports (WAI 2575)
- Academic research on Māori health equity, primary care access, and rural health workforce
- Waikato-Tainui and Te Tiratū statements
Unverifiable Claims: Identities of anonymous philanthropists remain unknown. Government refused to disclose under OIA. University of Waikato declined to comment.
Limitations: Full Detailed Business Case remains partially redacted. Exact financial arrangements between Waikato-Tainui and the University are not public.
Tools Used: Web search, document analysis, source verification via active research protocols.
All citations hyperlinked directly to source documents where available. No synthetic data generated.